Prostate Health
Imaging and Diagnosis of Prostate Cancer
Prostate HealthProstate Cancer
Traditionally, men with elevated PSA would require transrectal ultrasound-guided prostate biopsy to look for any prostate cancer. However, transrectal approach has a 1-2% chance of severe infection, and the biopsy procedure may also be prone to sampling error.
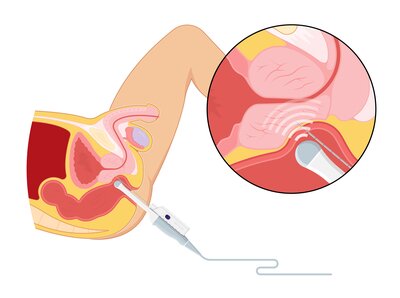
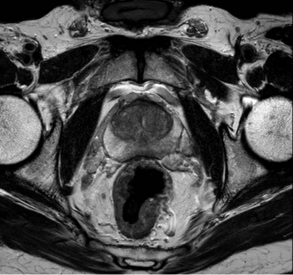
Recently, there have been a lot of advances in prostate cancer diagnosis. For men with elevated PSA, a MRI scan can be arranged to look for any tumours or suspicious lesions within the prostate gland. The MRI images can be fused into the ultrasound image during prostate biopsy, and targeted biopsy of the prostatic tumour can be performed. This will increase the accuracy of the biopsy procedure. On the other hand, if the MRI scan shows a completely normal prostate gland, prostate biopsy may also be safely avoided.
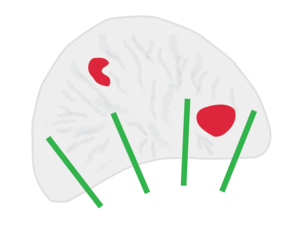
Conventional transrectal prostate biopsy requires puncture of the rectal wall, and bacteria within the rectum may enter the body and result in infection. In order to reduce the risk of infection, transperineal prostate biopsy can be performed. The perineum will first be disinfected during the procedure, and the perineal skin will be punctured in order to sample tissue from the prostate gland. The rectal wall remains intact during the whole prostate biopsy procedure, therefore bacteria within the rectum would not be able to enter the bloodstream. In recent years, transperineal prostate biopsy has gained increasing interest and adoption globally.
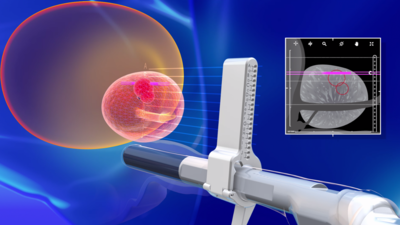
For patients with confirmed prostate cancer, it is important to look for any distant metastasis before deciding on the appropriate treatment. PSMA PET-CT scan is an accurate imaging for staging prostate cancer. In patients with localized disease, curative treatment such as robotic surgery, radiotherapy and focal therapy can be considered. In patients with metastatic prostate cancer, medical treatment such as hormonal therapy and chemotherapy may be considered.
Information about the different types of prostate cancer treatment can be found here.














